

 Call Us:
+91 8800015905
Call Us:
+91 8800015905

 Book an Appointment
Book an Appointment
 Locate us on Google Map
Locate us on Google Map
Subscribe to our alerts and receive regular healthcare information.
The Centre of Excellence in Orthopaedics and Joint Replacement is a state of the art facility at Aakash Healthcare; considered among the best orthopaedic hospitals in Delhi. The Centre provides systemic treatment and care for all orthopaedic complications and joint issues. Aakash is the top orthopaedic hospital in Dwarka, and some of Delhi’s best orthopaedic surgeons are available for any kn.....
The department of Neurosciences at Aakash Healthcare's delivers comprehensive Diagnostic and Therapeutic Neurology services around the clock, following evidence-based practices that follow internationally accepted guidelines. Our emergency services are provided round the clock for the diagnosis and treatment of neurological crises such as Status Epilepticus, Stroke, and Neuromuscular Weakness, .....
In contemporary times cancer care has experienced a paradigm shift and is all about comprehensive care, which requires commitment, expertise and a strong spirit. The Oncology team at Aakash Healthcare Super Speciality Hospital brings together the brightest minds in surgical & Medical Oncology.
.....
The term "cardiology" is derived from the Greek words "cardia" (heart) and "logy" (study of). Cardiology deals with disorders that affect the heart and even other parts of the circulatory system. This field includes the diagnosis and treatment of congenital heart defects, heart failure, valvular heart disease, coronary artery disease and electrophysiology. These and many other cardiac diseases .....
The department specializes in preventing, diagnosing and treating liver and gastrointestinal tract disorders. These include the diseases of liver, stomach, gall bladder, pancreas, esophagus, small and large intestine.The department offers state of art endoscopy procedures, 24 x7 gastrointestinal bleed management, foreign body removal and management of all gastrointestinal and liver emergencies .....
The liver is a digestive organ found only in vertebrates that detoxifies various metabolites, synthesizes proteins, and produces biochemicals required for digestion and growth. It is a cone shaped dark reddish-brown organ situated in the upper right quadrant of the abdominal cavity, beneath the diaphragm and on top of the stomach, right kidney, and intestines.
.....
In present day Chronic Kidney Disease is considered as a major medical problem and a silent killer worldwide. The Department of Renal Sciences and Kidney Transplantation is dedicated to provide the highest quality care for patients with renal disorders. Our multidisciplinary team of Nephrologists, Urologists and Transplant experts work together to provide comprehensive care for patients with ac.....
Aakash Healthcare, Department of Ophthalmology & Refractive Surgery has well-known eye physicians and surgeons and provides comprehensive care for eyes. We diagnose and treat various eye conditions every day, including many that are rare or complex. We offer a complete range of eye care services, from routine eye examination to surgery. We have state-of-the-art technologies and a vastly exp.....

Aakash MomMe is a specially curated program for the to-be and new moms, a unique concept, and the first of its kind in Dwarka . This program comprises full-fledged support plans for women before and during pregnancy, baby’s birth, and post-natal care. The entire program cycle is supported by doctors, nurses, educators, physiotherapists, psychologists, yoga trainers, and other speciality docto.....
Minimal access surgery also known as laparoscopy surgery is a means of performing surgeries through a small (keyhole) incision instead of large cuts. During the surgery, the surgeons introduce a telescope with a tiny video camera through the small incision to the targeted part of the body and operate it by viewing it on a high-resolution TV monitor. In traditional open surgery, Surgeons are una.....

Diet and Exercise often fail to treat people with extreme and excessive obesity effectively. Bariatric /weight loss/obesity surgery is performed to help such individuals lose weight. Bariatric surgery (weight loss surgery) aims to restrict food intake due to hormonal effects and decrease the absorption of food in the stomach and intestines. A reduction in the amount of calorie absorbed enables .....

Knee replacement surgery, also known as knee arthroplasty, can relieve pain and restore function in severely damaged knee joints. The procedure involves removing damaged bone and cartilage from your thighbone, shinbone, and kneecap and replacing it with a prosthesis made of metal alloys, high-grade plastics, and polymers.
The most common reason for knee replacement surgery is to relieve.....
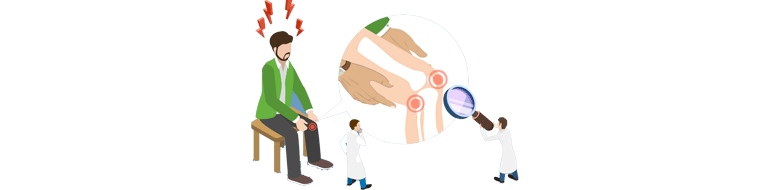
A Reconstruction of the ACL, or anterior cruciate ligament is a surgery meant to restore stability and strength to the knee for stability; after a knee ligament has been torn. The remnants of the torn ligament are removed and replaced with another ligament from the patient’s body or with tissue from a cadaver.
.....
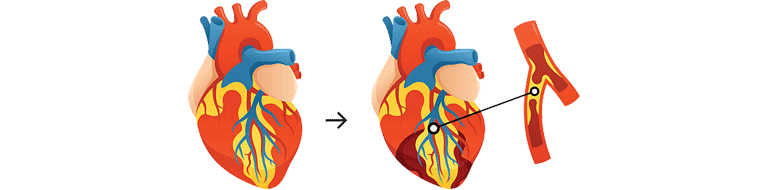
CABG is required whenever the arteries of the heart get blocked due to coronary artery disease and is done under full general anesthesia.
Idea of CAGB is to re-establish the blood supply to blocked arteries and it gives long term relief to the patients with very less chance of any reintervention.
.....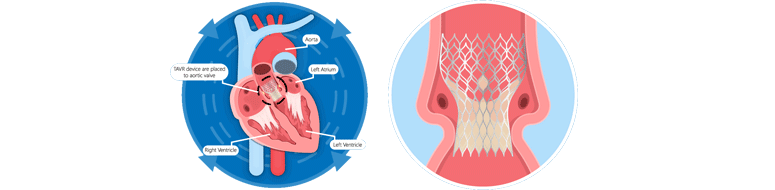
Transcatheter Aortic Valve Implantation (TAVI) also known as Transcatheter Aortic Valve Replacement (TAVR), is the replacement of the diseased aortic valve of the heart through the blood vessels in the leg (as opposed to the valve replacement by open heart surgery). The artificial valve is delivered via one of the several assess methods: Transfemoral (in the upper leg), Transapical (through the.....
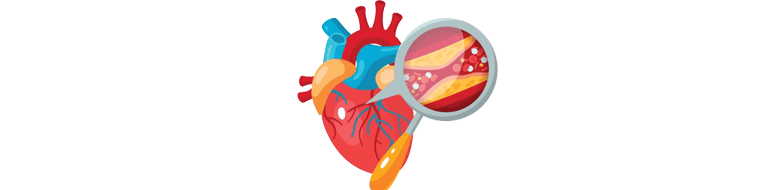
An angioplasty is a surgery that is essentially done to open blood vessels that supply blood to the heart, these blood vessels are also called coronary arteries. This is done as an emergency procedure mostly and is often performed immediately after a person suffers a heart attack. Almost 5 lakh people get coronary angioplasty done every year in India, and this figure is only going to rise accordin.....

Advances in cardiac science have proven to be a boon for patients suffering from end-stage heart disease. The good news is that an LVAD, or Left Ventricular Assist Device, is a lifesaver for patients who are waiting for a heart transplant. With advancements in science and technology, mechanical hearts have proven to be an excellent option for both heart failure patients and heart doctors. Raisi.....

When kidneys fail, toxic products, acid and fluid accumulates in body which effects other major organs like heart, brain and lungs leading to multi organ failure. There are two types of treatment presently available for failed kidneys – Dialysis or kidney transplantation. Kidney transplant offers no doubt is the best modality of treatment option for patients with kidney failure as it has show.....

Exercise and diet alone often fail to treat people with extreme and excessive obesity effectively. Bariatric surgery is performed to help such individuals lose weight. Bariatric surgery aims to restrict food intake due to hormonal effects and decrease the absorption of food in the stomach and intestines. A reduction in the amount of calory absorbed enables patients to lose weight and reduce obe.....
.png)
 The Centre of Excellence in Orthopaedics and Joint Replacement is a state of the art facility at Aakash Healthcare; considered among the best orthopaedic hospitals in Delhi. The Centre provides systemic treatment and care for all orthopaedic complications and joint issues. Aakash is the top orth.....
The Centre of Excellence in Orthopaedics and Joint Replacement is a state of the art facility at Aakash Healthcare; considered among the best orthopaedic hospitals in Delhi. The Centre provides systemic treatment and care for all orthopaedic complications and joint issues. Aakash is the top orth.....
.png)
 The department of Neurosciences at Aakash Healthcare's delivers comprehensive Diagnostic and Therapeutic Neurology services around the clock, following evidence-based practices that follow internationally accepted guidelines. Our emergency services are provided round the clock for the diagnosis a.....
The department of Neurosciences at Aakash Healthcare's delivers comprehensive Diagnostic and Therapeutic Neurology services around the clock, following evidence-based practices that follow internationally accepted guidelines. Our emergency services are provided round the clock for the diagnosis a.....
,_Hematology_Bone_Marrow_Transplant_(BMT).png)
 In contemporary times cancer care has experienced a paradigm shift and is all about comprehensive care, which requires commitment, expertise and a strong spirit. The Oncology team at Aakash Healthcare Super Speciality Hospital brings together the brightest minds in surgical & Medical Oncology......
In contemporary times cancer care has experienced a paradigm shift and is all about comprehensive care, which requires commitment, expertise and a strong spirit. The Oncology team at Aakash Healthcare Super Speciality Hospital brings together the brightest minds in surgical & Medical Oncology......
.png)
 The term "cardiology" is derived from the Greek words "cardia" (heart) and "logy" (study of). Cardiology deals with disorders that affect the heart and even other parts of the circulatory system. This field includes the diagnosis and treatment of congenital heart defects, heart failure, valvular .....
The term "cardiology" is derived from the Greek words "cardia" (heart) and "logy" (study of). Cardiology deals with disorders that affect the heart and even other parts of the circulatory system. This field includes the diagnosis and treatment of congenital heart defects, heart failure, valvular .....
.png)
 The department specializes in preventing, diagnosing and treating liver and gastrointestinal tract disorders. These include the diseases of liver, stomach, gall bladder, pancreas, esophagus, small and large intestine.The department offers state of art endoscopy procedures, 24 x7 gastrointestinal .....
The department specializes in preventing, diagnosing and treating liver and gastrointestinal tract disorders. These include the diseases of liver, stomach, gall bladder, pancreas, esophagus, small and large intestine.The department offers state of art endoscopy procedures, 24 x7 gastrointestinal .....

 The liver is a digestive organ found only in vertebrates that detoxifies various metabolites, synthesizes proteins, and produces biochemicals required for digestion and growth. It is a cone shaped dark reddish-brown organ situated in the upper right quadrant of the abdominal cavity, beneath the d.....
The liver is a digestive organ found only in vertebrates that detoxifies various metabolites, synthesizes proteins, and produces biochemicals required for digestion and growth. It is a cone shaped dark reddish-brown organ situated in the upper right quadrant of the abdominal cavity, beneath the d.....

 In present day Chronic Kidney Disease is considered as a major medical problem and a silent killer worldwide. The Department of Renal Sciences and Kidney Transplantation is dedicated to provide the highest quality care for patients with renal disorders. Our multidisciplinary team of Nephrologists.....
In present day Chronic Kidney Disease is considered as a major medical problem and a silent killer worldwide. The Department of Renal Sciences and Kidney Transplantation is dedicated to provide the highest quality care for patients with renal disorders. Our multidisciplinary team of Nephrologists.....
.png)
 Aakash Healthcare, Department of Ophthalmology & Refractive Surgery has well-known eye physicians and surgeons and provides comprehensive care for eyes. We diagnose and treat various eye conditions every day, including many that are rare or complex. We offer a complete range of eye care servi.....
Aakash Healthcare, Department of Ophthalmology & Refractive Surgery has well-known eye physicians and surgeons and provides comprehensive care for eyes. We diagnose and treat various eye conditions every day, including many that are rare or complex. We offer a complete range of eye care servi.....

 Aakash MomMe is a specially curated program for the to-be and new moms, a unique concept, and the first of its kind in Dwarka . This program comprises full-fledged support plans for women before and during pregnancy, baby’s birth, and post-natal care. The entire program cycle is supported by do.....
Aakash MomMe is a specially curated program for the to-be and new moms, a unique concept, and the first of its kind in Dwarka . This program comprises full-fledged support plans for women before and during pregnancy, baby’s birth, and post-natal care. The entire program cycle is supported by do.....

 Minimal access surgery also known as laparoscopy surgery is a means of performing surgeries through a small (keyhole) incision instead of large cuts. During the surgery, the surgeons introduce a telescope with a tiny video camera through the small incision to the targeted part of the body and ope.....
Minimal access surgery also known as laparoscopy surgery is a means of performing surgeries through a small (keyhole) incision instead of large cuts. During the surgery, the surgeons introduce a telescope with a tiny video camera through the small incision to the targeted part of the body and ope.....

 Diet and Exercise often fail to treat people with extreme and excessive obesity effectively. Bariatric /weight loss/obesity surgery is performed to help such individuals lose weight. Bariatric surgery (weight loss surgery) aims to restrict food intake due to hormonal effects and decrease the abso.....
Diet and Exercise often fail to treat people with extreme and excessive obesity effectively. Bariatric /weight loss/obesity surgery is performed to help such individuals lose weight. Bariatric surgery (weight loss surgery) aims to restrict food intake due to hormonal effects and decrease the abso.....

 Knee replacement surgery, also known as knee arthroplasty, can relieve pain and restore function in severely damaged knee joints. The procedure involves removing damaged bone and cartilage from your thighbone, shinbone, and kneecap and replacing it with a prosthesis made of metal alloys, high-gra.....
Knee replacement surgery, also known as knee arthroplasty, can relieve pain and restore function in severely damaged knee joints. The procedure involves removing damaged bone and cartilage from your thighbone, shinbone, and kneecap and replacing it with a prosthesis made of metal alloys, high-gra.....

 A Reconstruction of the ACL, or anterior cruciate ligament is a surgery meant to restore stability and strength to the knee for stability; after a knee ligament has been torn. The remnants of the torn ligament are removed and replaced with another ligament from the patient’s body or with tissue.....
A Reconstruction of the ACL, or anterior cruciate ligament is a surgery meant to restore stability and strength to the knee for stability; after a knee ligament has been torn. The remnants of the torn ligament are removed and replaced with another ligament from the patient’s body or with tissue.....

 Coronary angiography and angioplasty.
Peripheral angiography and angioplasty of the neck, leg, arm and kidneys.
EP study - diagnostic and ablation.
.....
Coronary angiography and angioplasty.
Peripheral angiography and angioplasty of the neck, leg, arm and kidneys.
EP study - diagnostic and ablation.
.....

 CABG is required whenever the arteries of the heart get blocked due to coronary artery disease and is done under full general anesthesia.
Idea of CAGB is to re-establish the blood supply to blocked arteries and it gives long term relief to the patients with very less chance of any reinter.....
CABG is required whenever the arteries of the heart get blocked due to coronary artery disease and is done under full general anesthesia.
Idea of CAGB is to re-establish the blood supply to blocked arteries and it gives long term relief to the patients with very less chance of any reinter.....

 Transcatheter Aortic Valve Implantation (TAVI) also known as Transcatheter Aortic Valve Replacement (TAVR), is the replacement of the diseased aortic valve of the heart through the blood vessels in the leg (as opposed to the valve replacement by open heart surgery). The artificial valve is delive.....
Transcatheter Aortic Valve Implantation (TAVI) also known as Transcatheter Aortic Valve Replacement (TAVR), is the replacement of the diseased aortic valve of the heart through the blood vessels in the leg (as opposed to the valve replacement by open heart surgery). The artificial valve is delive.....
 An angioplasty is a surgery that is essentially done to open blood vessels that supply blood to the heart, these blood vessels are also called coronary arteries. This is done as an emergency procedure mostly and is often performed immediately after a person suffers a heart attack. Almost 5 lakh peop.....
An angioplasty is a surgery that is essentially done to open blood vessels that supply blood to the heart, these blood vessels are also called coronary arteries. This is done as an emergency procedure mostly and is often performed immediately after a person suffers a heart attack. Almost 5 lakh peop.....

 Advances in cardiac science have proven to be a boon for patients suffering from end-stage heart disease. The good news is that an LVAD, or Left Ventricular Assist Device, is a lifesaver for patients who are waiting for a heart transplant. With advancements in science and technology, mechanical h.....
Advances in cardiac science have proven to be a boon for patients suffering from end-stage heart disease. The good news is that an LVAD, or Left Ventricular Assist Device, is a lifesaver for patients who are waiting for a heart transplant. With advancements in science and technology, mechanical h.....

 When kidneys fail, toxic products, acid and fluid accumulates in body which effects other major organs like heart, brain and lungs leading to multi organ failure. There are two types of treatment presently available for failed kidneys – Dialysis or kidney transplantation. Kidney transplant offe.....
When kidneys fail, toxic products, acid and fluid accumulates in body which effects other major organs like heart, brain and lungs leading to multi organ failure. There are two types of treatment presently available for failed kidneys – Dialysis or kidney transplantation. Kidney transplant offe.....

 Exercise and diet alone often fail to treat people with extreme and excessive obesity effectively. Bariatric surgery is performed to help such individuals lose weight. Bariatric surgery aims to restrict food intake due to hormonal effects and decrease the absorption of food in the stomach and int.....
Exercise and diet alone often fail to treat people with extreme and excessive obesity effectively. Bariatric surgery is performed to help such individuals lose weight. Bariatric surgery aims to restrict food intake due to hormonal effects and decrease the absorption of food in the stomach and int.....






All You Need to Know About H3N2 Virus...
Dr. Akshay Budhraja

Clean Hands, Safe Hands: The Importance of Hand Hygiene...
Dr. Sahil Kapoor

Understanding Thalassaemia: Symptoms, Causes and Treatment...
Dr. Roshan Dikshit
Robotic Knee Replacement Surgery vs Conventional Knee Replac...
Dr. Aashish Chaudhry